The Federal Bureau of Prisons' (BOP) stated mission is to protect society by confining offenders in the controlled environments of institutions and community-based facilities that are safe, humane, cost efficient, appropriately secure, and that provide work and other self-improvement opportunities to assist offenders in becoming law-abiding citizens. The mission of the BOP Pharmacy Services is to “provide access for inmates to quality, necessary, and cost–effective drug care consistent with community standards.”
As of July 2005, the BOP consisted of 106 institutions, 6 regional offices, a central office, 2 staff training centers, and 28 community corrections management offices. The BOP is currently responsible for the custody and care of approximately 182,000 federal offenders.
The BOP is faced with a significant challenge in providing adequate and cost effective medical care to inmates because of the rising federal inmate population the increasing cost of health care, as shown in Figure 1.
| FIGURE 1. | THE BOP ANNUAL PERCENT INCREASE IN HEALTH CARE COSTS AND POPULATION |
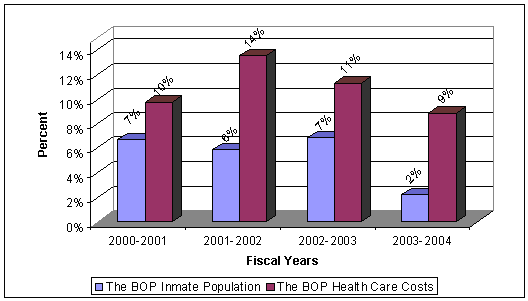 | |
| Source: Data provided by the BOP | |
Over the past 5 years, the BOP's inmate population has increased by 23 percent, from 123,141 in FY 2000 to 152,023 in FY 2004. The BOP's total health care costs for treating inmates increased from $412.65 million in FY 2000 to $623.52 million in FY 2004, an average annual increase of about 11 percent. During that same period, the BOP's costs for prescription medications and related supplies increased an average of 23 percent annually from $22.51 million in FY 2000 to $50.73 million in FY 2004. Additionally, the cost of prescription medications and related supplies has continued to account for a growing share of the BOP's total health care costs, rising from 5.5 percent in FY 2000 to 8.1 percent in FY 2004.
According to a Department of Health and Human Services report, the United States spends more on health care than any other industrialized nation.9 Health care costs account for a significant and increasing portion of the United States economy. In 1980, health care costs comprised only 9 percent of the Gross Domestic Product; however, by 2002 health care costs had increased to 15 percent. Additionally, from 1999 to 2002, health care costs increased an average of 8 percent annually, while the Gross Domestic Product only increased an average of 4 percent.
Health care costs consist of many different components. In 2002 the three largest components were hospital care (31 percent), physician and clinical services (22 percent), and prescription medications (11 percent). Of all these components, prescription medication costs have grown at the fastest rate, increasing by 167 percent from 1995 to 2002, as illustrated in Figure 2.
| FIGURE 2. | ANNUAL PERCENT INCREASE IN HEALTH CARE COSTS |
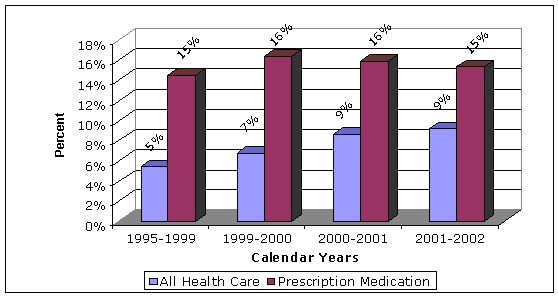 | |
| Source: Department of Health and Human Services, Center for Disease Control and Prevention, National Center for Health Statistics, Health, United States, 2004 | |
Two significant factors related to the rise in prescription medication costs are increased prices and increased usage. From 1995 to 2002 the Consumer Price Index for prescription medications and medical supplies increased by 35 percent, while the Consumer Price Index for the United States as a whole increased by only 18 percent. Additionally, the number of individuals reporting that they took at least one prescription medication in the month prior to the survey increased from 39 percent during the period from 1988 to 1994, to 44 percent during the period from 1999 to 2000. The survey also found that during the same periods, the number of individuals reporting that they took 3 or more prescription medications in the month prior to the survey increased from 12 percent to 17 percent.10
The BOP Health Services Division
The BOP Health Services Division consists of over 3,000 health care professionals including physicians, nurses, dentists, pharmacists, and mid level practitioners, of which 750 are United States Public Health Services Commissioned Officers. The Health Services Division provides a broad range of services to inmates, from routine patient care to surgery. These include dental, pharmacy, laboratory, radiological, and psychiatric services. The BOP Pharmacy Services Division is administered under the Health Services Division, whose mission is to “provide necessary medical, dental, and mental health services to inmates by a professional staff, consistent with acceptable community standards.11
As of February 2005, the BOP Pharmacy Services Division consisted of over 160 pharmacist positions, of which 133 are currently filled. About 120 BOP pharmacists are Public Health Services Commissioned Officers.12
The responsibilities of the BOP pharmacists include:
- tracking the controlled substances inventory;
- safeguarding controlled substances;
- ordering and receiving prescription medications;
- reviewing prescriptions for contraindications (e.g., potential negative interactions with other prescriptions and an inmate's medical condition);
- providing fellow practitioners with drug information, such as drug recalls, and drug interactions;
- filling prescriptions;
- monitoring an inmate's prescription medication usage to minimize waste and providing practitioners with information that helps treat inmates effectively, thereby ensuring that an inmate is taking the medication as prescribed;
- counseling patients;
- conducting clinics on diabetes, hypertension, mental health, and monitoring the treatment of infectious diseases;
- attending rounds with physicians; and
- providing discharge counseling.
The BOP is comprised of six major types of institutions, each of which generally have pharmacies: (1) Medical Referral Centers (medical centers), (2) Federal Correctional Institutions (FCIs), (3) United States Penitentiaries (USPs), (4) Metropolitan Correctional Centers (MCCs), (5) Federal Detention Centers (FDCs), and (6) Federal Prison Camps (FPCs). The BOP medical centers provide acute medical services, including surgery, cancer treatment, and long-term care. Although there are only seven BOP medical centers, they account for the largest amount (37 percent) of the BOP's total prescription medication costs, as shown in Figure 3.13
| FIGURE 3. | THE BOP PRESCRIPTION MEDICATION COSTS BY INSTITUTION TYPE FOR FY 2004 |
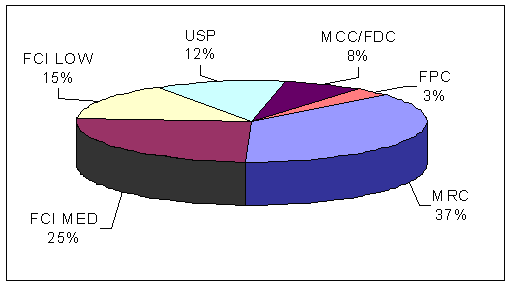 | |
| Source: The BOP Prescription Medication Cost Report | |
In FY 2004, the BOP spent $50.73 million on prescription medications and related supplies, representing an increase of 10 percent over the prior fiscal year. On average, there has been a 23-percent annual increase in the BOP's prescription medication costs since FY 2000. Furthermore, in FY 2004 the BOP spent a daily average of $0.92 per inmate on prescription medications. On average, the daily prescription cost per inmate has increased annually by 16 percent since FY 2000, as shown in Figure 4.
| FIGURE 4. | BOP DAILY PRESCRIPTION MEDICATION COSTS PER INMATE |
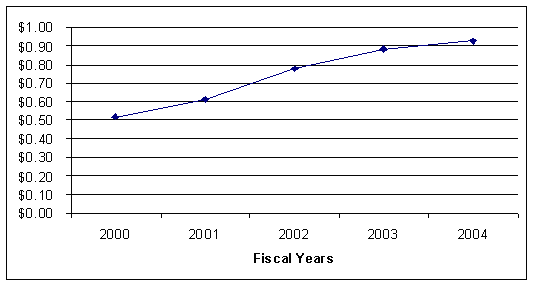 | |
| Source: Data provided by the BOP | |
The BOP attributes the increase in its prescription medication costs to the: (1) aging of inmates serving longer mandatory sentences, (2) increase in inmate population, and (3) increasing prices of prescription medications. However, we found that the average inmate age increased by 0.4 years from FY 2001 to FY 2004, which does not appear to support the BOP's assertion that the increase in prescription medication costs is caused, in part, by an aging inmate population. On the other hand, from FY 2000 to FY 2003 the increase in inmate population and consumer drug prices accounted for about 70 percent of the total increase in the BOP's prescription medication costs. From FY 2000 to FY 2003 the inmate population increased on average by 6 percent annually, while consumer prescription medication costs increased on average by 12 percent annually, as shown in Figure 5.
| FIGURE 5. | CHANGES IN PRESCRIPTION MEDICATION COSTS AND INMATE POPULATION14 |
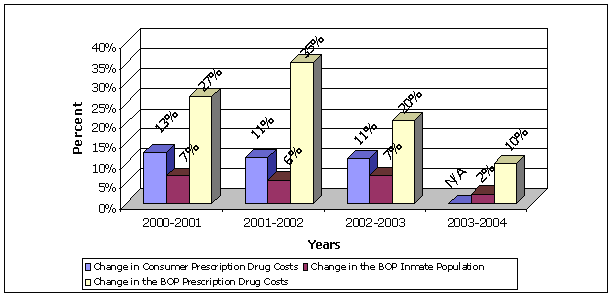 | |
| Source: Inmate population and prescription medication costs provided by the BOP; consumer costs obtained from the U.S. Statistical Abstract 2004-2005. | |
Treating inmates who test positive for Human Immunodeficiency Virus (HIV) and inmates requiring psychiatric care account for a significant portion of the BOP's total prescription medication costs. While the BOP reported that 1,677 inmates (or 1 percent) are HIV-positive, including 639 inmates with Acquired Immunodeficiency Syndrome (AIDS), the cost of prescription medications to treat HIV-positive inmates comprised 23 percent of the BOP's prescription medication costs in FY 2004. Additionally, the cost of HIV prescription medications increased by 14 percent from FY 2003 to FY 2004, while the HIV positive inmate population increased by only 5 percent. Prescription medication costs for treating inmates for psychological conditions also comprised 23 percent of the BOP's total prescription medication costs in FY 2004. As of March 2005, there were a total of 6,910 inmates who were being treated with one or more psychiatric medications within the BOP.15 In FY 2004, $23.49 million of the $50.73 million in total BOP prescription medication costs were related to HIV and psychiatric medications, as shown in Figure 6.
| FIGURE 6. | THE BOP PRESCRIPTION MEDICATION COSTS BY TYPE FOR FY 2004 (in millions) |
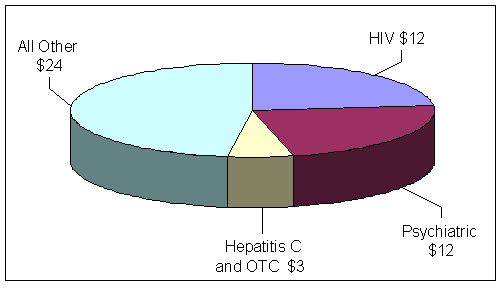 | |
| Source: Prescription medication costs provided by the BOP | |
The BOP utilizes the Federal Supply Schedule (FSS) for the majority of its prescription medication purchases. The FSS is a price catalog of over 23,000 prescription medications that are available for purchase by federal agencies. In addition to the FSS, the BOP utilizes specific contracts with prescription medication companies administered by the Veterans Administration (VA). The BOP purchases over 40 prescription medications through “Mandatory National Contracts” administered by the VA, which require that each institution buy specific prescription medication brands. These contracts provide the BOP with prices lower than the FSS, and include some frequently used medications, such as Tylenol®, Advil®, Aleve®, and Zocor®.
Current BOP Proposals to Reduce Prescription Medication Costs
According to the BOP, in an effort to reduce prescription medication costs, the BOP has implemented or plans to implement several changes to its health care and pharmacy programs including: (1) classifying institutions by the level of medical care required by inmates, (2) Central Fill and Central Processing of prescription medications, (3) use of an electronic medical records system, and (4) requiring inmates to pay for nonprescription medications.
Medical Level of Care Classifications
The BOP is reclassifying its institutions based on a four-level tier of medical care required by inmates. The BOP also plans to reorganize the staffing of its pharmacists to reflect the medical classification of its institutions.
- Level of Care 1 – Includes inmates who are generally healthy but may have limited medical or mental health conditions that can be easily managed by semi-annual clinical evaluations. This level consists of 10 institutions, of which 9 will not have an on site pharmacist. The BOP plans to restructure staffing for this level between January 2008 and December 2008.
- Level of Care 2 – Includes inmates who are stable but have chronic medical conditions requiring at least quarterly clinical evaluations but can still perform activities of daily living. This level consists of at least 60 institutions that will have 1 pharmacist on site, except for the Oklahoma Federal Transfer Center (FTC) which will continue to maintain 3 pharmacists.16 The BOP plans to restructure staff for this level between January 2009 and December 2011.
- Level of Care 3 – Includes inmates who are fragile outpatients requiring at least monthly clinical evaluations and who may have limitations in their ability to perform activities of daily living but do not require daily nursing care. The BOP has not decided the number of institutions or pharmacist staffing allocation for this level of care. The BOP plans to restructure staff for this level between January 2009 and December 2010.
- Level of Care 4 – Include inmates who require the services available at the six medical centers and who may require daily nursing care. The BOP has not decided the pharmacist staffing allocation for this level. The BOP plans to restructure staff for this level between January 2009 and December 2010.
Central Fill and Central Processing
To address concerns related to the rising cost of prescription medications, the BOP created the Pharmacy Workgroup (Workgroup). The Workgroup is comprised of 11 members representing many departments within the BOP, headed by the BOP Chief Pharmacist. Pursuant to an Executive Staff Paper dated April 30, 2004, the objectives of the Workgroup are to:
- control costs by consolidating prescription medications into a main inventory and buying the least expensive brand of generic medications; and
- establish an automated prescription medication fulfillment system that provides medications in a timely manner for all BOP institutions.
The Workgroup recommended that the BOP establish an Interagency Agreement with the Department of Veterans Affairs Centralized Mail Outpatient Pharmacy Center in Dallas, Texas, to fill prescription medications for BOP institutions. Through Central Fill, the onsite pharmacists at BOP institutions would review prescriptions for the following contraindications, as required by BOP policy:17
- drug to drug interactions,
- drug to disease interactions,
- drug to food interactions,
- therapeutic duplications,
- allergies,
- therapeutic appropriateness,
- appropriate dose,
- duration of therapy,
- adverse drug reactions, and
- final check of the prescription to ensure it contains the correct medication.
The pharmacists would then electronically transmit prescriptions to the VA. Once the order is received, the VA would fill the prescription via its automated system and mail it overnight to the BOP institutions. The institutions would receive the prescription medication the following morning and administer or dispense it to inmates.
The October 25, 2004, draft Interagency Agreement between the BOP and the VA states that Central Fill will “improve the cost efficiencies through economies of scale and clinical effectiveness of BOP Pharmacists.” The BOP expects the Level of Care 1, 2, and 3 institutions to use Central Fill for 95 percent of their prescriptions. Conversely, the BOP expects the Level 4 institutions and FDCs to use Central Fill for 50 percent of their prescriptions because of the unique missions of these institutions.
The Workgroup cited several benefits related to its Central Fill proposal, including improving drug inventory management, reducing redundancies, eliminating the majority of bulk stock from institutions, reducing errors through the use of barcode labels on prescriptions, and increasing the use of pharmacists in a clinical capacity. According to the BOP, increasing the use of its pharmacists in a clinical capacity would improve inmate medical care, reducing overall health care costs. Clinical pharmacy would require BOP pharmacists to:
- assist doctors with continuity of care to improve medication management;
- monitor, modify, and discontinue prescription medication therapy, as needed;
- order, perform, and evaluate laboratory tests; and
- conduct clinics to help inmates manage diseases, including diabetes, HIV, Hepatitis C, asthma, and others.
The BOP provided several reports illustrating the benefits of clinical pharmacy. According to a 2002 report in the American Journal of Health System Pharmacy, HIV clinics conducted by pharmacists improved patient compliance and care.18 The report also stated that the vast majority of pharmacists working in the clinics improved treatment effectiveness by 62 percent. Furthermore, according to a 2003 report in the Journal of American Pharmacists Association, a diabetes clinic run by pharmacists reduced the average direct medical cost per patient from $1,872 to $1,200 per year.19
The Workgroup also proposed the development of Central Processing, whereby institutions lacking an on site pharmacist could electronically transmit inmates' prescriptions to a central location where the BOP's pharmacists would review prescriptions for contraindications, and in turn, transmit them electronically to Central Fill. All BOP institutions would use Central Processing as a backup or during periods when an on site pharmacist was not available. BOP officials noted that one benefit from this proposal would be to reduce the need to hire contract pharmacists to assist when staff is on leave. The BOP estimates that Central Processing would save about $2 million a year, assuming that an average of 65 institutions use a contract pharmacist for 50 days a year at a rate of $80 per hour. However, the BOP has not conducted a formal cost-benefit analysis of the Central Processing proposal.
Figure 7 illustrates the relationships between the BOP's Levels of Care, Central Fill, and Central Processing proposals.
FIGURE 7. THE CENTRAL FILL AND CENTRAL PROCESSING
| [Image Not Available Electronically] |
| Source: BOP Pharmacy Staff |
- Level of Care 1 Institutions – The institution would transmit prescriptions to the Central Processing center using prescriber order entry. This is an electronic method by which prescriptions are entered into a computer system by the prescriber and sent to a central location for processing. A pharmacist at the Central Processing center would review the prescription for contraindications and then transmit the prescription electronically to Central Fill.
- Level of Care 2, 3, and 4 Institutions – The on site pharmacist at the institution would review prescriptions for contraindications during normal business hours and then transmit the prescriptions electronically to Central Fill. If the prescription is for an acute medication, the institution's pharmacist would order it directly from the prime vendor. During periods when the onsite pharmacist is not available, the institution would transmit prescriptions via prescriber order entry to Central Processing, which would then transmit the prescription electronically to Central Fill.
The BOP plans to implement Central Fill and Central Processing over the next 6 years. The BOP estimates that it will sign the Interagency Agreement for Central Fill with the VA by June 2006. Once the agreement is signed, the BOP estimates that it will take more than 3 years to fully implement the changeover to Central Fill. The BOP plans to implement Central Fill for the Level 1 institutions by December 2007, with all other institutions being implemented by December 2009.
Electronic Medical Records System
The development of an electronic medical records system is included as an objective in the BOP's 2005 Strategic Plan, which states, “Implement an electronic medical records system which incorporates all medical, psychiatric, psychological, and disability information about individual inmates. The electronic medical records system will incorporate information currently maintained separately in paper medical records, the Psychology Data System, the Correctional Institution Pharmacy System, and the SENTRY data base."20 In conjunction with the Central Fill and Central Processing proposals, the BOP is in the planning and development stages of implementing an electronic medical records system.
The electronic medical records system would provide pharmacists with the ability to access an inmate's medical information from any location, thus providing them with the ability to conduct a complete review of inmate prescriptions to check for any contraindications. In addition, the system would provide the capability for prescriber order entry, allowing other physicians to enter prescriptions into the system electronically. A recent study published by the Journal of the American Medical Association showed that computerized physician prescribing reduced errors by 80 percent.21
If the proposed electronic medical records system is not implemented, we would be concerned with the feasibility of implementing Central Processing, because it is unclear which level of information would be provided to pharmacists to conduct their review of the prescriptions for contraindications.
Over-the-Counter (OTC) Medications
In an effort to reduce the costs of prescription medications, the BOP issued the OTC Medication Program Statement on November 17, 2004.22 This statement outlines the requirements that each institution – other than medical centers – must follow when using OTC medications for the treatment of inmates. The BOP's OTC policy requires that inmates who complain about cosmetic, general hygiene issues, or symptoms of minor ailments should be referred to the commissary where they can purchase OTC medications with their own funds. If an inmate is considered indigent, that is, having less than a $6 average balance in their account for the last 30 days, then the institution can provide two OTC medications per week to the inmate.
In 2000, the Government Accountability Office (GAO) conducted a review of the health care costs at the BOP.23 It found that from FY 1990 to FY 1999 the average annual increase in BOP health care costs was about 8.6 percent. The GAO noted several BOP initiatives to help reduce health care costs, including cooperative agreements using VA contracts to purchase prescription medications. In the report, the BOP stated that this resulted in a $0.76 million annual savings for health care costs. The GAO report also stated that the BOP made progress in containing health care costs, but additional proposals would help to contain increasing costs. These proposals included the BOP implementing a co-payment for inmates and negotiating more cost-effective contracts with community hospitals.
The Department of Justice (DOJ) Office of the Inspector General (OIG) conducted this audit to evaluate the BOP Pharmacy Services. Our objectives were to:
- evaluate the BOP's efforts to reduce its increasing costs of prescription medications;
- assess whether the BOP ensures adequate controls and safeguards over prescription medications; and
- assess whether the BOP pharmacies are in compliance with applicable laws, regulations, policies, and procedures.
During the audit we conducted work at BOP headquarters and the 12 institutions shown in Figure 8.24
| FIGURE 8. BOP INSTITUTIONS AUDITED |
|
At each of the above institutions, we:
- reviewed documentation from FY 2002 to FY 2005 related to costs of prescription medications, lost or stolen controlled substances, investigations pertaining to the pharmacy and its staff, program and operational reviews, and access to the pharmacy;
- analyzed selected samples related to purchases, prescriptions, inventory, and disposal of controlled and noncontrolled substances from FY 2004 and FY 2005; and
- interviewed BOP officials, analyzed the use of OTC medications, and obtained information impacting the BOP's proposals to reduce the cost of prescription medications.
In addition, we analyzed the BOP's Central Fill and Central Processing proposals and conducted a survey of all BOP Pharmacists.
The details of the results of our audit are contained in the Findings and Recommendations section of this report. Additional information related to our audit appears in the Objectives, Scope, and Methodology section.
- Department of Health and Human Services, Center for Disease Control and Prevention, National Center for Health Statistics, Health, United States, 2004.
- Department of Heath and Human Services, National Center for Health Statistics, Health, United States, 2004.
- The BOP defines Mid-Level Practitioners as Physician Assistant Certified, Physician Assistant Non-Certified, and Nurse Practitioner.
- BOP Program Statement No. 6000.05, Health Services Manual, updated February 11, 2000.
- As of September 2005, the BOP was in process of reclassifying the medical center in Fort Worth, TX, to an FCI. As a result, when discussing the BOP's future actions we refer to six, rather then seven, medical centers.
- Due to the availability of data, the data for the Change in Consumer Prescription Drug Costs is based on the calendar year, while the Change in the BOP Inmate Population, and the Change in the BOP Prescription Drug Costs is based on fiscal year.
- This number does not include data from the Oklahoma FTC, the Rochester Medical Center, and the Beaumont Federal Correctional Complex because they do not use the same tracking program as the other BOP institutions.
- The Oklahoma FTC will not use Central Fill for its prescription medications because of the constant turnover of inmates at the facility. Consequently, there will be no change in its pharmacist staffing levels.
- BOP Program Statement No. P6360.01, Pharmacy Services, dated January 15, 2005.
- American Journal of Health-System Pharmacy, Issue 59(8) (2002).
- Journal of American Pharmacists Association, Issue 43(2) (2003).
- SENTRY is the BOP's primary on-line information system.
- Journal of the American Medical Association, “Leading Patient Safety Advocates Assess Progress in Reducing Medical Error Five Years After Landmark IOM Report,” (May 18, 2005).
- BOP Program Statement No. 6541.01, Over-the-Counter Medications, issued November 17, 2004.
- Government Accountability Office, Federal Prisons: Containing Health Care Costs for an Increasing Inmate Population (2000).
- We also visited the Englewood FCI, Colorado, to obtain background information; however, the Englewood FCI is not included in our audit results.