The Federal Bureau of Prisons (BOP) is responsible for confining federal offenders in prisons that are safe, humane, cost-efficient, and secure. As part of these duties, the BOP is responsible for delivering medically necessary health care to inmates in accordance with applicable standards of care.
As of November 29, 2007, the BOP housed 166,794 inmates in 114 BOP institutions at 93 locations.1 During FY 2007, the BOP obligated about $736 million for inmate health care. The BOP provides health care services to inmates primarily through: (1) in-house medical providers employed by the BOP or assigned to the BOP from the Public Health Service, and (2) contracted medical providers who provide either comprehensive care or individual services.
To control the rising cost of health care, since the early 1990s the BOP has implemented initiatives aimed at providing more efficient and effective inmate health care. The BOP’s on-going initiatives include assigning most inmates to institutions based on the care level required by the inmate, installing an electronic medical records system that connects institutions, implementing tele-health to provide health care services through video conferencing, and implementing a bill adjudication process to avoid costly errors when validating health care-related invoices. We include a discussion of these cost-cutting initiatives and the effect the initiatives have had on controlling inmate health care costs in the Findings and Recommendations section of this report.
OIG Audit Approach
The Department of Justice Office of the Inspector General (OIG) initiated this audit to determine whether the BOP: (1) appropriately contained health care costs in the provision of necessary medical, dental, and mental health care services; (2) effectively administered its medical services contracts; and (3) effectively monitored its medical services providers.
We performed audit work at BOP headquarters and at the following BOP institutions: the United States Penitentiary (USP) Atlanta (Georgia), USP Lee (Virginia), Federal Medical Center (FMC) Carswell (Texas), Federal Correctional Complex (FCC) Terra Haute (Indiana), and FCC Victorville (California). In addition, we surveyed the 88 BOP locations where we did not perform on-site work. The details of our testing methodologies are presented in the audit objectives, scope, and methodology contained in Appendix I.
This audit report contains 3 finding sections. The first finding discusses the BOP’s efforts to contain the growth of health care costs and to deliver necessary health care to inmates in a cost-effective manner. The second finding discusses the BOP’s administration of medical services contracts. The third finding discusses the BOP’s efforts to monitor its medical services providers, both in-house and contract staff.
Results in Brief
We found that the BOP has implemented or begun numerous cost containment initiatives since fiscal year (FY) 2000 that appear to have helped it contain inmate health care costs. Although the BOP generally did not maintain analytical data to assess the impact that the individual initiatives had on health care costs, our audit found that the BOP has kept the growth of inmate health care costs at a reasonable level compared to national health care cost data reported by the Departments of Health and Human Services and Labor.
However, we also determined that each of the BOP institutions we tested did not always provide recommended preventive health care to inmates. Our audit found that for almost half of the preventive health services we tested, more than 10 percent of the sampled inmates did not receive the medical service.
In addition, OIG audits of BOP medical contracts have found multiple contract-administration deficiencies, such as inadequate review and verification of contractor billing statements. Several of the contract-administration deficiencies appeared to be systemic. While the BOP had taken action to address individual deficiencies at local institutions, we also found that other BOP institutions lacked appropriate controls in the deficiency areas identified by prior OIG contract audits.
We also identified weaknesses in the BOP’s monitoring of health care providers. Specifically, the BOP: (1) did not develop agency-wide guidance to correct apparent systemic problems found during medical-related internal reviews and external audits; (2) did not provide health care providers with current authorization to practice medicine on BOP inmates through privileges, practice agreements, or protocols; (3) had not performed required initial and renewal peer reviews for providers; and (4) had not implemented an effective performance measurement system related to the provision of health care at BOP institutions.
In our report, we make 11 recommendations regarding the BOP’s provision of medical care for inmates. These recommendations include: establishing procedures to assess whether individual initiatives are cost-effective and producing the desired results; determining the necessity of performing medical services that generally were not performed by most BOP institutions; providing guidance and procedures to all BOP institutions for performing certain contract administration functions related to inmate health care; and ensuring that privileges, practice agreements, or protocols are established for all practitioners, as applicable.
The remaining sections of this Executive Summary describe in more detail our audit findings.
Cost Containment
Since FY 2000, the BOP has implemented or developed at least 20 initiatives designed to improve the delivery of health care to inmates, improve the administration and management of health care, and reduce or contain rising health care costs. As of December 2007, the BOP had implemented 11 of these initiatives and was in the process of implementing the remaining 9 initiatives.
In the following table, we provide a description of four of the BOP’s major initiatives. Appendix II contains a description of the 20 initiatives.
| Initiative | Description |
|---|---|
| Medical Designations Program | This initiative involves: (1) assigning each inmate a care level from 1 to 4, with 1 being the healthiest inmates and 4 being inmates with the most significant medical conditions; (2) assigning each BOP institution a care level designation from 1 to 4 based on the inmate care level that the institution is staffed and equipped to handle; (3) staffing each institution based on its designated care level; and (4) moving inmates between institutions to match each inmate’s care level to the care level of the institution. |
| Medical Staff Restructuring | Under this initiative, the BOP established staffing guidelines for Care Level 1, 2, and 3 institutions. Because institution staffing did not always match the care level staffing guidelines, the BOP had to move medical staff throughout the BOP to implement the guidelines. Institutions that had staff in positions contrary to the guidelines were required to either move the staff to another facility or reassign the staff to another authorized position in the facility. |
| Tele-medicine | This initiative involves the remote delivery of health care using telecommunications technologies such as video-conferencing. |
| Electronic Medical Records | This initiative involves automating the medical records for inmates. The initial system included the capability to: (1) track comprehensive history and physical examination information, (2) schedule inmate medical visits when required, and (3) track medical-related supplies and equipment issued to inmates. The BOP subsequently added a pharmacy module to the system to manage the medications provided to inmates. |
We attempted to determine the effect that the BOP’s initiatives had on inmate health care costs. However, while the initiatives had a primary or secondary purpose of reducing or containing health care costs, the BOP could not provide either preliminary cost-benefit analyses or any post-implementation analyses to identify costs reduced or contained by these initiatives. BOP officials believed that preliminary cost-benefit analyses had been performed, but said the documentation of the analyses was no longer available. As for post-implementation analyses, BOP officials told us that the BOP does not collect and maintain cost-related data that would allow it to analyze the cost-effectiveness of each of its health care initiatives. As a result, we recommend that the BOP collect cost-related data for each initiative and use the data collected to analyze whether the initiatives are providing the anticipated cost benefits.
Because the BOP did not maintain cost data for its health care initiatives, we were also unable to assess the impact of each initiative individually. Instead, we analyzed the overall effect of the BOP’s initiatives on total medical costs. We compared the BOP’s per capita health care costs for calendar years 2000 through 2006 to similar data reported by the Department of Health and Human Services (HHS) and the Department of Labor (DOL). We found that although the BOP experienced growth in excess of the HHS national average for medical costs and the DOL Consumer Price Index (CPI) for medical costs during some of the earlier years of our review period, the BOP’s growth rates since 2002 have declined significantly, even though the growth rates in the HHS national average and the DOL CPI have not. The following graph shows the results of our comparison.
Comparison of the Growth Rates of Health Care Costs for BOP HHS, and DOL Health Care Data for Calendar Years 2000 through 20062
[Image Not Available Electronically]
Source: BOP Office of Research and Evaluation, BOP Budget Execution
Branch, Department of Health and Human Services, and Department of Labor
The above comparison indicates that the BOP has been effective in containing the growth of health care costs.
Preventive Health Care
The BOP periodically develops program statements to disseminate policy on a variety of BOP programs. Appendix VI contains a brief description of the BOP program statements related to the provision of medical, dental, and mental health services to inmates.
The BOP has also established 16 clinical practice guidelines containing diagnostic procedures for specific medical areas, such as preventative health care, coronary artery disease, and hypertension. The Introduction section of this audit report contains a list of the 16 medical areas covered by the clinical practice guidelines. While the guidelines have not been incorporated into the BOP’s program statements as policy, the BOP Medical Director told us that BOP institutions are expected to provide the services in the guidelines to the inmates. The Medical Director also told us that the institutions have discretion in whether to follow the guidelines on a case-by-case basis. However, BOP institutions must request and receive approval from the Medical Director to not implement a specific guideline requirement.
To determine whether the institutions were providing expected medical services to inmates, we selected and tested specific medical services listed in the BOP’s Preventive Health Care Clinical Practice Guideline. We chose this particular BOP guideline because:
-
It addressed care for all inmates, instead of only inmates with specific illnesses;
-
It included diagnostic procedures for 9 of the 11 chronic conditions addressed in the other 15 guidelines;
-
It contained clearly defined medical services that could be reasonably tested;
-
Health promotion and disease prevention is a primary objective of the BOP’s efforts to contain costs; and
-
The BOP Medical Director told us that testing of the preventive health care guideline would provide useful information to the BOP because its per capita cost of providing health care should be reduced by implementing a good preventive health program, and he expects the institutions to provide the services contained in the guideline.
We specifically selected and tested 30 medical services contained in the preventive health care guideline, including whether: (1) inmates received a measles, mumps, and rubella vaccine; (2) inmates received a hepatitis A vaccine; (3) inmates received a cholesterol check in the last 5 years; (4) female inmates received a chlamydia test; and (5) female inmates received a bone density screening test.3
To perform our testing of the 30 medical services, we selected a sample of 1,110 of the 14,026 inmates assigned to 5 BOP locations as of March 24, 2007, as shown in the table below. Appendix IV contains an explanation of our sampling methodology.
Inmate Population and Inmates Sampled
| BOP Facility | Inmate Population as of March 24, 2007 |
Inmates Sampled |
|---|---|---|
| USP Atlanta (Georgia) | 2,494 | 251 |
| USP Lee (Virginia) | 1,808 | 133 |
| FCC Terra Haute (Indiana) | 3,343 | 249 |
| FMC Carswell (Texas) | 1,677 | 127 |
| FCC Victorville (California) | 4,704 | 350 |
| Totals | 14,026 | 1,110 |
For each inmate sampled, we reviewed the inmate’s medical record and determined whether the inmate received the 30 preventive services, as applicable. The 30 services were not applicable to all inmates sampled for reasons such as certain services applied to only female inmates, certain services were only for inmates over a certain age, and other services applied only if the inmate had certain risk factors. To validate our testing, we asked a Health Services Unit official at each of the facilities tested to confirm our results and ensure that we had not overlooked the provision of any service.
While the BOP guideline suggests that all inmates should receive the applicable services, we recognize that 100 percent compliance is unlikely given the movement of inmates between prisons, staffing shortages, and other reasons. Therefore, we noted a deficiency when 10 percent or more of the inmates for whom the service was applicable had not received it.
As demonstrated in the following two charts, the combined results for all 5 locations showed that for 16 of the 30 services tested, 90 percent or more of the inmates received the preventive service as appropriate. For the remaining 14 services, more than 10 percent of the sampled inmates did not receive the medical service.4 For example, 94 percent of the inmates who should have received a cardiovascular risk calculation had not received one in the last 5 years, as recommended by BOP guidelines. Additionally, 87 percent of the sampled inmates needing a measles, mumps, and rubella vaccine had not received this service.
Overall Results of the OIG’s Testing of
Medical Services Provided to Inmates5
| Medical Service Tested | Inmates Tested |
Yes | No |
|---|---|---|---|
| 1. Inmate medical history provided by inmate at intake | 1,044 | 99% | 1% |
| 2. Medical assessment completed by medical practitioner at intake | 1,044 | 99% | 1% |
| 3. New inmate tested for tuberculosis or previous test for transferred inmate confirmed, within 48 hours of intake | 1,043 | 99% | 1% |
| 4. Inmate received rapid plasma regain test during intake screening to test for syphilis | 403 | 92% | 8% |
| 5. Female inmate tested for chlamydia | 25 | 36% | 64% |
| 6. Female inmate received a measles/mumps/rubella vaccine | 128 | 81% | 19% |
| 7. Inmate received a complete physical within 14 days of intake | 1,044 | 95% | 4% |
| 8. Inmate received a pneumococcal vaccine | 93 | 74% | 23% |
| 9. Inmate received an annual influenza vaccine | 210 | 71% | 29% |
| 10. Inmate born after 1956 received a measles/ mumps/rubella vaccine | 932 | 13% | 87% |
| 11. Inmate received a tetanus vaccine in the last 10 years | 1,042 | 50% | 49% |
| 12. Inmate received a hepatitis A vaccine | 263 | 57% | 42% |
| 13. Inmate received a hepatitis B test or vaccine | 343 | 90% | 9% |
| 14. Inmate received a hepatitis C test | 267 | 91% | 8% |
| 15. Inmate received an HIV-1 test | 381 | 93% | 6% |
| 16. Inmate received an HIV-2 test | 130 | 98% | 2% |
| 17. Inmate received a tuberculosis test in the past year | 869 | 98% | 2% |
| 18. Inmate received a chronic care evaluation in the last 6 months | 339 | 98% | 2% |
| 19. Inmate received a cholesterol check in the last 5 years | 678 | 71% | 29% |
| 20. Inmate received a cardiovascular risk calculation in the last 5 years | 402 | 6% | 94% |
| 21. Inmate received a fasting plasma glucose test in the last 3 years | 324 | 84% | 12% |
| 22. Inmate received a current blood pressure check | 1,043 | 96% | 4% |
| 23. Inmate received a current body mass index calculation | 1,036 | 12% | 88% |
| 24. Inmate received a fecal occult blood test | 189 | 46% | 54% |
| 25. Inmate received a vision screening test | 58 | 93% | 7% |
| 26. Inmate received a hearing screening test | 35 | 51% | 49% |
| 27. Inmate received an abdominal ultrasound test | 6 | 100% | - |
| 28. Female inmate received a papanicolaou test (PAP smear) | 142 | 99% | 1% |
| 29. Female inmate received a current mammogram | 89 | 100% | - |
| 30. Female inmate received a bone density screening test | 8 | 38% | 62% |
We found that the institutions either did not usually provide or were inconsistent in providing 18 of the 30 medical services we tested. For example, the cardiovascular risk calculation was rarely performed in the 5 institutions we tested. Moreover, as shown in the chart below, we found that the percentage of applicable inmates not receiving a cholesterol check within the past 5 years ranged from 68.1 percent at USP Lee to 8.3 percent at FMC Carswell. This disparity in medical service provision indicates a need for better BOP headquarters oversight and guidance.
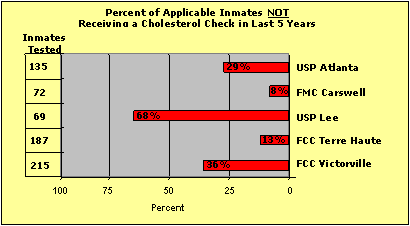
| Source: OIG testing of BOP medical records |
We asked officials at each of the five locations for an explanation of why some services were not provided to a significant number of inmates. FMC Carswell medical officials declined our requests for an explanation, stating that BOP headquarters would provide a response after we issued our report. The following are examples of explanations given to us by officials from the other four locations.
-
The vaccine was not always available to give to the inmate.
-
The officials believed that a requirement applicable to all inmates only applied to women.
-
The officials used alternative methods in place of certain services.
-
The officials considered the service unnecessary.
-
The inmates failed to return the test cards.
-
The officials overlooked the requirement.
-
The officials believed the procedures were too costly.
-
Staffing inadequacies and scheduling constraints precluded the officials from providing the service.
Another factor that could have contributed to expected medical services not being provided consistently is that four of the five institutions had not fully implemented the Primary Care Provider Teams (PCPT) as required by the BOP’s patient care policy. Under the PCPT model, each inmate is assigned to a medical team of health care providers and support staff who are responsible for managing the inmate’s health care needs. The PCPT model is designed to provide inmates with better and more consistent medical care because the inmate is examined by the same provider team each time the inmate requires medical attention. If the same provider team examines an inmate during each visit, the inmate should be less likely to miss some services because the provider team would be familiar with the services previously provided to the inmate. According to the BOP’s Preventive Health Care Clinical Practice Guideline, the most efficient and cost-effective way to implement the guideline is to assign appropriate responsibilities to each PCPT member. However, we found that only the FMC Carswell had implemented the PCPT concept. The other four institutions had not fully implemented the PCPT concept primarily because of limited staffing.
Contract Administration
The BOP relies on contractors to provide a substantial amount of medical services to inmates, and the OIG periodically performs audits of the BOP’s comprehensive medical contracts. From August 2004 through March 2007, the OIG issued nine audit reports on BOP medical contracts. Appendix X contains a summary of these audits. Eight of the nine OIG contract audits identified major internal control deficiencies. The deficiencies included management control weaknesses pertaining to calculating medical service discounts, reviewing and verifying contractor invoices and billing statements, paying bills, and managing the overall administration of the contracts. The audits indicated several of the weaknesses were systemic, such as:
-
Six of the contract audits found weaknesses in verifying and reviewing the accuracy of invoices for medical services provided by the contract providers.
-
Five of the contract audits found weaknesses in obtaining supporting documentation for contractor billing statements.
-
Four of the contract audits found errors in the Medicare or diagnostic-related groups discount rates.
-
Three of the contract audits found that the contractor did not provide the services stated in the contract, and the contractor’s performance reports were either inaccurate or submitted in an untimely fashion.
The audits usually found that the identified weaknesses were attributable to the lack of written procedures and other internal controls. As of November 2007, the BOP had implemented corrective actions for all the recommendations in seven of the nine contract audits. For the other two audits the BOP agreed to take corrective actions concerning our recommendations, and those actions were either completed or in progress as of November 2007. In response to six of the nine audits, the BOP strengthened management controls by establishing written procedures for processing and monitoring contract medical claims. However, these actions were limited to correcting the deficiencies only at the institutions where the deficiencies were found.
As part of this larger audit of BOP medical services we tested whether the BOP as a whole had strengthened controls related to the deficiencies identified in the contract audits. We interviewed BOP officials at the five BOP locations tested. For the remaining 88 BOP locations, we sent survey questionnaires and asked whether the institutions had established management control procedures for their comprehensive medical contracts, including:
-
reviewing contractor invoices for accuracy,
-
ensuring contractor invoices are supported by adequate documentation,
-
ensuring that invoice discounts are properly applied,
-
ensuring that contractor performance reports are complete and accurate, and
-
ensuring that contractor timesheets are verified by a BOP employee.
We found that up to seven BOP institutions lacked critical controls for certain contract administration functions, and about half the institutions with critical controls had not documented the procedures associated with the controls.
Our analysis of survey responses found that 77 of the 88 BOP institutions surveyed had comprehensive medical service contracts. Generally, officials at each institution responded that they had established internal control procedures for administering its contracts. However, we found that about half the institutions had not formalized these procedures in written policy for the controls we tested, as noted in the chart below.
Controls Established by BOP Institutions for
Comprehensive Medical Services Contracts
| Contract Administration Function |
Number of Institutions | |||
|---|---|---|---|---|
| Procedures not Established |
Procedures Established |
Procedures Established but not Written |
Percent of Established Procedures not Written |
|
| Reviewing contractor invoices for accuracy | 1 | 76 | 39 | 51% |
| Ensuring contractor invoices are supported by documentation | 3 | 74 | 36 | 49% |
| Ensuring invoice discounts are properly applied | 7 | 70 | 34 | 49% |
| Ensuring contractor performance reports are complete and accurate | 2 | 75 | 35 | 47% |
| Ensuring contractor timesheets are verified by a BOP employee | 2 | 75 | 43 | 57% |
The lack of written procedures increases the risk that appropriate controls will not be fully and consistently implemented, especially when staff assignments and duties change. We found during our medical service contract audits that the lack of management controls resulted in questionable payments to contractors, and we believe it is possible based on these results that similar errors may have occurred for medical contracts in other BOP facilities. It is essential that the BOP strengthen controls over administering its contracts by providing guidance and procedures to its institutions to help ensure that systemic deficiencies are corrected BOP-wide.
Monitoring Health Care Providers
The BOP has established numerous mechanisms to monitor its health care providers. Some of the mechanisms include:
-
conducting internal program reviews to determine whether each institution is properly implementing BOP policies, including policies related to inmate health care;
-
granting clinical privileges and establishing practice agreements and protocols based on health care providers’ qualifications, knowledge, skills, and experience;6
-
conducting peer reviews of health care providers to review the current knowledge and skills of the providers; and
-
requiring each institution to accumulate and report performance data on a quarterly basis for specific health-related areas.
The primary purpose of these monitoring mechanisms is to improve the quality and efficiency of health care delivered to inmates by:
(1) identifying and correcting deficiencies in the provision of health care, and
(2) authorizing duties for health care providers commensurate with their skills and capabilities.
Our audit found that the BOP corrects deficiencies at the institutions at which deficiencies are found, but generally does not develop and issue agency-wide guidance to correct systemic deficiencies found during internal program reviews. We also found that the BOP allowed several health care providers to practice medicine without valid authorizations. Additionally, providers had not had their medical practices evaluated by a peer as required by BOP policy. Moreover, while institutions were accumulating and reporting data on health-related performance measures, the BOP does not develop agency-wide corrective actions when the performance is below target levels. These issues are summarized in the following sections.
Program Reviews
The BOP’s Program Review Division monitors health care services provided to inmates through periodic reviews generally conducted once every 3 years, or more frequently if significant problems are identified. From FYs 2004 to 2006, the Program Review Division conducted 110 health care program reviews at 88 BOP locations. We analyzed the 110 review reports and determined that 40 of the 110 reviews found medical services deficiencies. The Program Review Division required institutions to certify completion of corrective actions for the deficiencies identified.
The Program Review Division also prepared quarterly summary reports of the program reviews. The summary reports identified the most frequent deficiencies found during the reviews and were distributed to the Chief Executive Officers within the BOP, including the Health Services Division Medical Director. However, a senior Health Services Division official told us that the BOP probably would not change its policy when program reviews find problems in a certain area, but it might provide training to improve staff knowledge and compliance. The official told us that the Health Services Division relies on the BOP Regional Offices and institutions to correct identified problems.
We analyzed the 40 BOP reviews and found that 25 different medical services were not provided to inmates and 14 of the 25 deficiencies were noted at multiple institutions. For example, as shown in the table on page 32 of this report, the Program Review Division found inmates with chronic care conditions who were not monitored as required at 16 institutions. Also, the reviews found inmates who were not monitored for psychotropic medical side effects at 11 institutions. We believe the BOP should use the program summary reports prepared by the Program Review Division to develop or clarify agency-wide guidance on systemic weaknesses and issue the guidance to all BOP institutions.
Privileges, Practice Agreements, and Protocols
In the provision of inmate health care, BOP institutions use the following health care providers.
Licensed independent practitioners are medical providers authorized by a current and valid state license to independently practice medicine, dentistry, optometry, or podiatry.
Non-independent practitioners are graduate physician assistants (certified or non-certified), dental assistants, dental hygienists, nurse practitioners, and unlicensed medical graduates.
Other practitioners are those not included in the above categories and include clinical nurses and emergency medical technicians.
To improve the quality of medical care that these medical providers provide to inmates, the BOP: (1) grants clinical privileges to licensed independent practitioners based on the practitioner’s qualifications, knowledge, skills, and experience; (2) establishes practice agreements between its licensed independent practitioners and its non-independent practitioners, such as mid-level practitioners; (3) establishes protocols that must be followed by other health care providers; and (4) performs periodic peer reviews of all providers who function under clinical privileges or practice agreements.
The BOP grants clinical privileges to its in-house and contracted practitioners. Clinical privileges are the specific duties that a health care provider is allowed to provide to BOP inmates. BOP policy states that clinical privileges can be granted for a period of not more than 2 years, and that newly employed physicians can be granted privileges for a period of not more than 1 year. Practitioners are prohibited from practicing medicine within the BOP until they have been granted privileges to do so by an authorized BOP official.
The individual institutions establish practice agreements between their licensed independent practitioners and their non-independent practitioners. Practice agreements delegate specific clinical or dental duties to non-independent practitioners under a licensed independent practitioner’s supervision and are valid for no more than 2 years. Non-independent practitioners are prohibited from providing health care within the BOP until a practice agreement has been established.
The BOP’s other health care providers, such as clinical nurses and emergency medical technicians, must work under protocols approved by licensed independent practitioners. A protocol is a plan for carrying out medical-related functions such as a patient’s treatment regimen.
To determine whether the BOP maintained current privileges, practice agreements, and protocols for each of its practitioners, we included relevant questions in our survey questionnaire sent to 88 BOP institutions. Based on the responses to our questionnaires, we identified 134 practitioners out of 1,536 (9 percent) who were allowed to provide medical services to BOP inmates without current BOP privileges, practice agreements, or protocols.
BOP Medical Practitioners without Current
Privileges, Practice Agreements, or Protocols
| Type of Authorizing Document |
Practitioners Requiring Authorizing Document |
Practitioners without Authorizing Document |
Percent without Authorizing Document |
|---|---|---|---|
| Privileges | 680 | 72 | 11% |
| Practice Agreement | 466 | 42 | 9% |
| Protocol | 390 | 20 | 5% |
| Totals | 1,536 | 134 | 9% |
Based on this data, it is apparent that BOP officials do not fully understand the type of authorization different health care providers should receive, or ensure that the health care providers have them.
Allowing practitioners to provide medical care to inmates without current privileges, practice agreements, or protocols increases the risk that the practitioners may provide medical services without having the qualifications, knowledge, skills, and experience necessary to correctly perform the services. In addition, the BOP could be subjected to liability claims by inmates if improper medical services are provided by these practitioners.
Peer Reviews
BOP policy requires that BOP health care providers have a periodic peer review. A peer is defined as another provider in the same discipline (physician, dentist, mid-level practitioner, or others) who has firsthand knowledge of the provider’s clinical performance. The peer review should evaluate the professional care the provider has given using a sample of the provider’s primary patient load and comment on specific aspects of the provider’s knowledge and skills, such as actual clinical performance, judgment, and technical skills. BOP health care providers who are privileged or working under a practice agreement must have at least one peer review every 2 years. Each Clinical Director, Chief Dental Officer, and Clinical Psychiatrist must also have a peer review at least once every 2 years.
In our survey questionnaire sent to 88 BOP institutions, we requested the last peer review date for all providers with privileges or practice agreements. For the 891 such providers, the responses to the questionnaire indicated that 430 (48 percent) had not received a current peer review. We asked BOP officials about the lack of peer reviews. The officials responsible for more than half of the non-current peer reviews did not provide an explanation. The officials responsible for the remaining non-current peer reviews cited the following reasons.
-
The officials rely on contractors to do peer reviews.
-
The officials believed that the peer review requirement did not apply to mid-level practitioners, dental assistants, or dental hygienists.
The officials relied on performance reviews instead of doing the required peer reviews.
Without a current peer review, the BOP has a higher risk of providers giving inadequate professional care to inmates, thus subjecting the BOP to formal complaints and lawsuits. Also, if inadequate professional care goes undetected, the providers may not receive the training or supervision needed to improve the delivery of medical care.
Performance Measures
The BOP has also established national performance measures for health care to include annual targets or goals for management of:
(1) hypertension, (2) cholesterol, (3) diabetes, (4) HIV, (5) tuberculosis, (6) asthma, (7) breast cancer, (8) cervical cancer, and (9) pregnancy. The BOP institutions voluntarily report results for these performance measures to the BOP Health Services Division on a quarterly basis.
In our survey questionnaire, we asked institution officials if they had completed the performance measure calculations for the nine performance measures for calendar year 2004 through the first quarter of calendar year 2007. The following table details the 99 responses from officials at the 88 BOP locations.7
| Performance Measure Calculations Completed for Calendar Year |
BOP Response | |||
|---|---|---|---|---|
| Yes | No | Not Applicable |
No Response |
|
| 2004 | 59 | 28 | 10 | 2 |
| 2005 | 77 | 14 | 4 | 4 |
| 2006 | 87 | 11 | 0 | 1 |
| 2007 (1st Quarter) | 90 | 7 | 1 | 1 |
Based on the responses, the number of institutions not completing the performance measure calculations decreased each year since 2004. However, when asked why the calculations were not always completed, BOP officials usually could not provide an explanation and said that the person who was responsible for completing the calculations was no longer at the institution. The officials who did provide an explanation usually attributed not completing the performance measure calculations to staffing shortages.
We also analyzed the performance measure reports from the BOP and found that the institutions often did not meet the target levels established for the nine target goals. For the nine health care performance measures we tested, we found that the institutions reported performance below the target level for more than 20 percent of the quarters reported for seven of the nine performance measures. For example, for the clinical management of lipid level measure, 79 institutions reported results for 723 quarters between January 1, 2004 and March 31, 2007. The results reported were below the target level for 437 (60 percent) of the quarters reported. In another example related to the clinical management of diabetes, the 79 institutions reported below target level performance for 285 (39 percent) of the 729 quarters reported.
We discussed with BOP Health Services Division officials their review of and response to the performance reports. The officials told us that they review the reports, perform a trend analysis, and summarize the results in the Office of Quality Management’s Annual Report. However, the officials also told us that institution participation in reporting the performance measures is voluntary and they do not develop agency-wide corrective actions when the performance is below target levels. We believe it is essential that the BOP take corrective actions when performance is below targets to help ensure that inmates are provided adequate medical care.
In addition, we found that instructions are needed to help ensure performance data are consistently accumulated and reported. The BOP did not provide institutions with instructions on accumulating and reporting such data. According to a BOP Health Services Division official, the institutions are inconsistent in how they accumulate and report performance data. If this is the case, the summary data compiled by the BOP may not be meaningful. This BOP Health Services Division official also told us that because of the inconsistencies in data reported, the BOP is developing a training program to educate institution staff on how to properly accumulate and report performance data. According to the Chief of the BOP’s Quality Management Section, a meeting was held in December 2007 with the institution Health Services Administrators to discuss the collecting of national performance measure data. Another meeting is planned for January 2008 to discuss with Regional Medical Directors any adjustments needed to the performance measurement system.
Conclusion and Recommendations
In general, we found that in comparison to other national health care cost indices, the BOP was successful at containing the growth of inmate health care costs. However, our audit concluded that the BOP could make improvements to help ensure that: (1) inmates are provided recommended preventative medical care, (2) contract administration deficiencies are addressed BOP-wide, and (3) monitoring of medical service providers is strengthened. If the deficiencies we noted in these areas are not corrected, we believe the BOP could experience:
-
higher costs for providing health care,
-
decreases in the quality of health care,
-
a higher number of medical-related complaints from inmates, and
-
greater liability for lack of adequate medical care.
To assist the BOP in improving medical care for inmates, we made 11 recommendations to the BOP. These recommendations include:
(1) establishing procedures for collecting and evaluating data for current and future health care initiatives to assess whether individual initiatives are cost-effective and producing the desired results; (2) reviewing the medical services that the OIG and the BOP’s Program Review Division identified as not always provided to inmates and determining whether the medical services are necessary or whether the medical service requirement should be removed from the program statements or clinical practice guidelines, as appropriate; (3) providing additional guidance to the institutions to ensure that medical services deemed necessary are provided to the inmates, (4) providing additional guidance and procedures to all BOP institutions for performing certain contract administration functions; (5) developing and issuing agency-wide guidance to correct systemic deficiencies found during internal program reviews; and (6) ensuring that privileges, practice agreements, or protocols are established for all practitioners, as applicable.
Appendix V contains a list of the Bureau of Prisons (BOP) institutions. The BOP housed an additional 33,354 inmates in privately managed, contracted, or other facilities. For the purposes of this audit, we focused on the medical care provided to inmates housed in BOP facilities.
The BOP’s, the Department of Health and Human Services’ (HHS) and the Department of Labor’s (DOL) per capita health care medical costs are not fully comparable. The BOP’s medical per capita costs include costs for services not included in HHS’s and the DOL’s per capita medical costs and vice versa. Even though the costs are not fully comparable between the three measures, we believe the cost measures are sufficiently similar for comparison purposes. The HHS national average cost data was obtained from the HHS report, National Health Expenditures Aggregate, Per Capita Amounts, Percent Distribution, and Annual Percent Change by Source of Funds: Calendar Years 2005 – 1960 (January 2007). An updated report showing cost data for 2006 was not available.
The percentages in the chart are based on the number of inmates for whom the service was applicable.
Some percentages in the chart total less than 100 percent because documentation was not available to determine if the service was performed for some inmates.
Clinical privileges and practice agreements authorize the specific clinical or dental duties that health care providers may provide to BOP inmates.
The total responses (99) to our survey questions was more than the 88 BOP locations surveyed because 6 of the locations surveyed submitted separate responses for the 17 BOP institutions at the locations. Performance measures were not applicable for some institutions primarily because the institutions are new and were not active for the years tested.